Did you know?
- COPD is the 4th leading cause of death worldwide - 75% of those affected remain untreated.
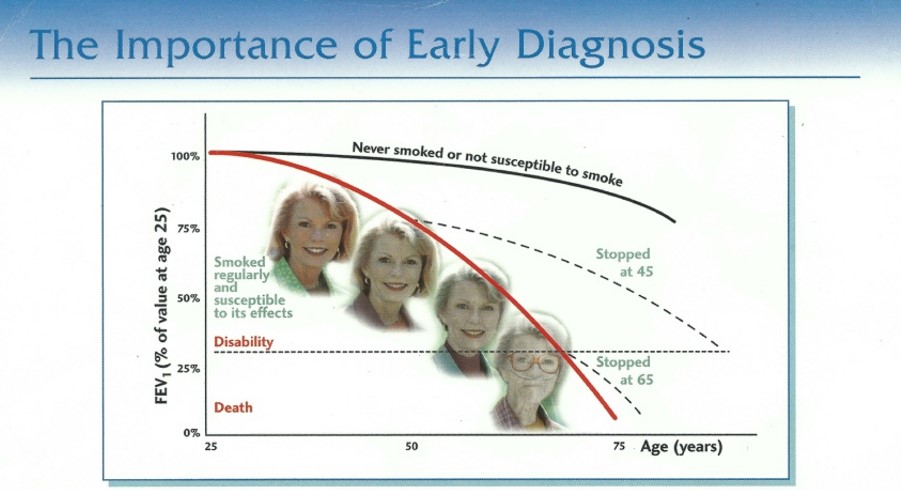
- Most people with COPD are not diagnosed until the disease is well advanced.
- The sooner COPD is diagnosed, the better the outcome.
- Smoking is the most common cause of COPD. (All smokers & former smokers ages 40 and over, should have a lung function test).
What is COPD?
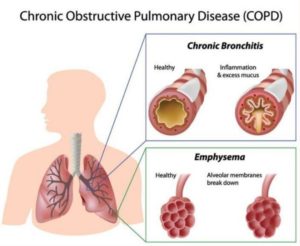 Chronic Obstructive Pulmonary Disease (COPD) is a disease that makes it difficult for air to move into and out of your lungs. It causes the airways of the lungs to be inflamed and become ‘obstructed’ or blocked. Drawing a breath can be a difficult frightening struggle.
Chronic Obstructive Pulmonary Disease (COPD) is a disease that makes it difficult for air to move into and out of your lungs. It causes the airways of the lungs to be inflamed and become ‘obstructed’ or blocked. Drawing a breath can be a difficult frightening struggle.
COPD includes bronchitis and emphysema.
- Bronchitis means the airways are inflamed and narrowed and often produce excess sputum.
- Emphysema affects the air sacs at the end of the airways, causing them to lose function and trap air.
Both these conditions make it harder to move the air in and out of your lungs as you breathe, causing a lack of oxygen in the lungs.
COPD is caused by cigarette smoking, occupational exposure to dusts, and possibly outdoor air pollution.
Diagnosis of COPD
COPD is a disease that progresses slowly. Lung damage, however, can develop long before you notice any symptoms. The sooner COPD is diagnosed, the sooner you can start treatment and stabilize your symptoms.
Doctors can tell if you have COPD by measuring the airflow of your lungs. Through a simple breathing test called spirometry, a machine measures your total lung capacity and how much air you can breathe out in one second, a reading called forced expiratory volume (FEV).
If your lungs are obstructed, you will not be able to breathe out as much air as someone without lung obstruction.
The GOLD international guidelines advise Spirometry as the gold standard for accurate diagnosis of COPD and repeatable measurement of lung function.
According to these results your doctor will diagnose your level of COPD
There are 4 stages or grades of COPD
- Stage 1 Early
- Stage 2 Moderate
- Stage 3 Severe
- Stage 4 Very Severe
Your doctor will assign grades to these 4 things:
- How severe your current symptoms are.
- Your spirometry results
- The chances that your COPD will get worse
- The presence of other health problems.
Are you at Risk of COPD?

Managing My COPD
Quit Smoking
 Quitting smoking will slow the progression of COPD.
Quitting smoking will slow the progression of COPD.
The first step in preventing and treating COPD is to quit smoking. If you have COPD and you continue smoking, your lungs will get worse. The best way to prevent COPD from developing or to stop it from getting worse is to quit smoking.
It is NEVER TOO LATE to quit smoking (contact Open Airways for information about smoking cessation programs).
Vaccination
COPD patients have a higher risk of requiring hospitalization due to the flu. COPD patients should receive a flu shot once a year. Consult your doctor to see if you need a pneumonia vaccine. COVID???
Exercise
Exercise can help keep you from deterioration physically and improve your ability to carry out daily activities. Benefits include improved breathing, improved endurance of leg muscles, and improved quality of life.
- Singing can be a great exercise for your lungs, join a choir and socialise at the same time!
- Buy yourself some sneakers and get walking, simple and effective, the best exercise.
- Talk to your doctor or physiotherapist for guidance on exercise.
Control Your Breathing
COPD can cause airways to collapse when you breathe out (exhale), trapping stale air. This leaves less room in your lungs for fresh air to enter. When this happens you are likely to feel short of breath.
Techniques such as Pursed-lip breathing keeps airways open longer during exhalation. This helps release trapped air from your lungs and allows fresh air to come in.
Practice pursed-lip breathing while you are resting so you can use this technique when you are feeling short of breath. Use this technique during exercise or activities that causes you to be short of breath. However, this technique also may be used at anytime. Link here to pop-out of pursed breathing. (below)
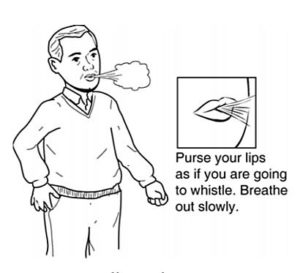 Breathe in or inhale through your nose at a normal rate and depth. Feel your lungs fill with air.
Breathe in or inhale through your nose at a normal rate and depth. Feel your lungs fill with air.- Purse your lips together as if you are going to whistle or play a flute.
- Breathe out or exhale slowly and gently through your mouth, keeping your lips pursed. The time it takes to exhale should be 2 to 3 times longer than the time you inhale. Do not force air out.
- Adjust your breathing rhythm and the amount you purse your lips to increase your comfort.
Here are some additional tips for controlling breathing:
- Breathlessness quick reference guide (from Asthma Foundation New Zealand) https://www.asthmafoundation.org.nz/assets/documents/2021-ARFNZ-breathlessness-quick-reference-2_RLR_2021.pdf
- Additional tool guides (from Asthma Foundation New Zealand)
https://www.asthmafoundation.org.nz/resources/breathlessness-strategies-for-copd
 Controlling Anxiety
Controlling Anxiety
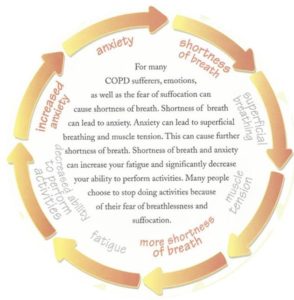
Controlling your anxiety is very important when preventing and decreasing shortness of breath.
The less you do, the less you are in shape, the more anxious you will become, and short of breath.
This is a vicious cycle, that needs to be broken.
Additional Tips for Living with COPD
- Don’t smoke
- Avoid unhealthy air quality, keep away from dust, fumes and smoke. Avoid fresh air sprays and plug-ins and household cleaning chemicals especially aerosols. Avoid products with fragrances. Do not use scented candles or essential oil diffusers.
- Open windows every day, turn on a fan or use a hand-held fan.
- Clean without chemicals using microfiber cloths, damp mops and a vacuum cleaner.
- Get annual flu shot and ask your doctor about the pneumonia and other vaccines too.
- Eat a healthy diet, see a dietitian if you need to lose weight or have difficulty eating due to severe breathlessness. (Contact Island Nutrition – [email protected] phone: 2954082)
- Practice your breathing exercises every day
Keep moving – at whatever stage of COPD you must keep moving, walking at whatever pace is comfortable for you is the simplest form of exercise.
COPD Medications
Inhalers may be prescribed by your doctor to reduce your symptoms of COPD. Be sure to take all medications the way your doctor instructs you. Different medications may be prescribed to manage COPD. Review medications ANNUALLY with your doctor.
Bronchodilators - either short or long-acting form the mainstay of drug therapy for COPD. They help to open up the airways and reduce shortness of breath.
Short-acting bronchodilator
If you only get short of breath occasionally, your doctor may prescribe a short-acting bronchodilator. This will provide quick relief lasting 4-6 hours. These inhalers should be used with a spacer.
Long-acting bronchodilator
If you are breathless daily your doctor may prescribe a bronchodilator which can last 12 -24 hours
There are two types of long-acting bronchodilators, LAMA (long-acting anti-muscarinic) or LABA (long-acting beta agonist). Most people with COPD will benefit from taking both kinds. They may come in separate inhalers or in combination inhalers.
Steroid Inhalers - Some people need to use inhaled steroids as part of their treatment. Steroids reduce inflammation in the airways to help improve breathing in patients. They may reduce the risk of flare-ups. Your doctor will most likely prescribe a combination inhaler, with one or two bronchodilators and a steroid.
Do you know how to use your inhaler?
If you are unsure how to use your inhalers contact Open Airways nurse at [email protected]
Or follow these links for videos on how to use your inhaler:
Antibiotics help fight bacterial infections and may be required in addition to COPD medication during an exacerbation (flare-up).
Oxygen Therapy can help prolong the life of some patients with severe COPD. Oxygen therapy can reduce breathlessness and improve mental function in COPD patients. Oxygen concentrators are available locally from Medical House and Lighthouse Medical and should be covered by all local health insurance policies.
If you are without insurance Open Airways may be able to help, contact [email protected]
Managing COPD Flare-ups
A flare-up or exacerbation is when your COPD symptoms worsen and become severe.
Signs of a flare-up
- Your breathlessness gets worse
- You are coughing more
- You produce more sputum
- There is a change in colour and consistency of your sputum
Flare-ups may be triggered by an infection. Be aware of changes in your symptoms if you get a cold.
Make sure you have a plan of action agreed with your doctor, so you know what to do when your symptoms worsen.
You may have a rescue pack of medications (antibiotics or steroid tablets or both) that you keep at home. Notify your doctor if you need to start your rescue pack.
Many people can be treated at home for a flare-up, but you may need to go to hospital if your symptoms are severe.
Call 9-1-1 or go to Emergency immediately if:
- You are struggling to breathe or have sudden shortness of breath
- Your chest feels tight or heavy
- You have a pain that spreads to your arms, back, neck and jaw
PREVENT LUNG INFECTIONS Flare-ups of COPD are sometimes caused by bacterial infections in the lungs. Wash your hands regularly and limit your exposure to sick people to reduce your risk of infection.
COPD self-management plans
Self-management of your COPD with support from your doctor or nurse will help give you control of your condition.
A self-management plan is designed to help you understand your COPD and show you how to manage your daily symptoms. It will guide you to know when to change your treatment, and how to deal with flare-ups.
Please talk to your doctor about your COPD action plan.
Helpful link to self-management plans: https://www.blf.org.uk/support-for-you/copd/your-copd-self-management-plan
